#lollies nz online
Text

Get the Best Online Pricing On Rainbow Confectionery in NZ | Stock4Shops
Explore a variety of Rainbow Confectionery products at Stock4Shops, including rainbow lollies, jelly and gummies. Indulge in these delicious treats sourced directly from the original manufacturers.
Plus, enjoy complimentary fast delivery within New Zealand when you spend over $300 on your purchase. Your order will arrive at your doorstep within just 48 hours.
0 notes
Text
FREEBIES
Every purchase comes with the following freebies :
Mental Health Awareness sticker.
Lollies ranging from lollipops, chocolates and mints.
Random Sticker
Wax Seal Sample card (depending on availability)
Every month, one lucky person may be able to receive a free product. If you would like to receive a free product from us, please read through the guidelines to check if you are eligible.
Must have 10,000+ followers on Instagram/Tiktok.
Must upload a dedicated post and story of the free product on 2 social media platforms within 3-5 days once received. (Instagram, Tiktok, Facebook or even Youtube if applicable).
Must tag us on the post.
Must be residing either on New Zealand or Australia.
Guidelines will be strictly followed. Please consider that we are only a small business and cannot afford to give out free products without anything in exchange. However, we would want to be able to grow more to be able to do so in the future. But for now, we would appreciate your support and understanding regarding the rules for a free product/s.
If you think that you are eligible or would like to ask any question regarding this matter, please don't hesitate to contact us at [email protected].
Subject must be titled : Royal Freebies.
State the reason why you would like to receive the product.
Provide NZ/AUS address you would like the product to be sent to.
List of at least 2 (or more) social media platforms and your username/s.
Proof of follower counts (screenshot, we will be checking it ourselves too).
Once approved, you will receive an email as confirmation and will need to sign a document stating that you will be uploading a dedicated post and story on your platforms.
Please note that this post is an extension/related to our online store at www.royallavendershop.com
1 note
·
View note
Text
Cadbury Dairy Milk with Pascall Clinkers

SPECIAL EDITION
Bought at Pak n Save for $2.99
170g block
Clinkers candy pieces 8%
Cocoa Solids 27%
Milk Solids 24%
Sugars per 25g serving size is 14.5g
Made in Tasmania Australia
We don't always buy these novelty type blocks, but Joni remembers Clinkers with fondness. If you have never tried them, they are like a hard Eskimo lolly with a bit more fruity flavor punch, covered in chocolate. They have different fruit flavors, and you didn't know what flavor you would get until you bit into them.
In New Zealand you can't find them in the supermarkets anymore, but I did find you could buy them online from the Remarkable Sweet Shop NZ.
It smells like Clinkers and it tastes like a mix of different flavored Clinkers. The Clinkers add a nice crunch and the balance of Clinkers and chocolate is quite good. The aftertaste? CLINKERS!
This block was actually a bit of fun. Don't buy it for a serious chocolate tasting experience, but for the yummy Clinker bits, and a bit of nostalgic fondness.


0 notes
Link
Sweetporium NZ is Aotearoa's resident online candy store! Shop a huge range of old school, Kiwi, and American candy in NZ at awesome prices. Get pick and mix sweets shipped to your doorstep, or give the gift of a delicious candy gift box.
0 notes
Text
Week 1.2
Inequality In New Zealand

Health Inequalities In New Zealand

Social and Economic Determinants of Health

Oral Health Research
Jones, Nicholas. Time for Free Dental Care? The Huge Expense of Going to the Dentist | Health Central. 4 Mar. 2019, https://healthcentral.nz/time-for-free-dental-care-the-huge-expense-of-going-to-the-dentist/.
Desperate Kiwis are queuing at hospital pain clinics because they can’t afford the dentist - and health bosses are not backing free dental care.
“Waitemata District Health Board wants a “comprehensive dental service for all New Zealanders”, its chief executive confirmed
The position comes amidst growing concern among health workers about people who can’t afford hefty dentist’ bills and live in chronic pain as a result, with some resorting to gruesome “DIY dentistry”.
There are long queues at hospital pain clinics for temporary fillings for teeth extractions, people turning up at emergency departments because of dental pain.
Members discussed whether the health boards should call on the government to provide subsidised or free dentistry.
Waitemata DHB chief executive, Dr dale Bramley, told the meeting the Ministry of Health was “already considering how the dental service could be included in the public health service, and that the DHB boards should support”.
A resolution was passed by the committee recommending the DHBs “support comprehensive dental care access for all New Zealanders as part of the public health system”
Grant Pollard, the ministry’s group manager for population health, denied any current work on possible changes to publicly-funded dental care.
Any more to provide more subsidised or free dental care would carry a huge cost. Currently, about $198 million a year is spent on oral health services, with most covering universal services for children and teenagers.
Kiwis without enough money live in chronic pain that affects work, quality of life and mental and wider health
Gum disease increases the risk of heart disease, and poor oral health increases the chances of bacterial infection in the bloodstream
Adults must pay the full cost, and bills can run into thousands of dollars.
Hamilton dentist Dr Assil Russell launched a petition for subsidy for dental care for at-need people and an increase in the age for free dental care to 20 years.
Russell’s charity Receive a Smile has treated almost 10,000 patients free of charge, including those with bad infections, and broken and rotting teeth.
Currently, Government-funded dental work for adults is limited to emergency care for pain and infection relief, and work and income grants for those on a low income and who are in serious pain and need urgent treatment. Dental care is also given to a small number of hospital inpatient and work needed after accidents are funded by ACC.
The NZ Dental Association wants more subsidised care for people on low incomes - but not universal access saying such a step would likely cost more than the annual budget of large DHBs
Helen Clark tweeted Jacinda Ardern, Winston Peters and Social Development Minister Carmel Sepuloni: “Time for a major government initiative on the right to dental care. NZ makes hospital care free - why not a right to dental care?’
The cost of dental work:
Examination only: $76
Single tooth extraction $229
Each additional tooth taken: $138
Root Filling $735
One surface filling $153
Composi te crown $408
Hygienist - half hourly rate: $110
Full upper and lower dentures $2557 (the average fee charged by NZ Dental Association members, according to the association’s 2018 fee survey)
Broadbent, Jonathan. High Cost Means More than Half of NZ’s Young Adults Don’t Access Dental Care | Health Central. 30 May 2019, https://healthcentral.nz/high-cost-means-more-than-half-of-nzs-young-adults-dont-access-dental-care/.
In New Zealand wealth determines dental health
Inequalities in untreated tooth decay are wider in New Zealand than in Australia, Canada or the United States.
The latest NZ Health Survey run annually by the MOH reported that cost prevents an estimated 15 per cent of NZ adults (just over half million) from seeing a GP about a medical problem and nearly 7 per cent (around a quarter million) from filling a prescription. For dentistry, cost stopped 44 per cent of adults (around 1.6 million) from accessing care. In the young adult age group, this was over half the population.
Adult dental health care is a neglected health policy issue
The risk for dental problems is determined in early childhood and can be intergenerational
Those born into disadvantaged families go on to have greater rates of tooth decay as adults.
Young adulthood is when incomes are often at their lowest but untreated dental decay is at its highest
Conventional wisdom has it that the best approach to reducing inequalities is to educate the public but that doesn't work. To address social inequalities we need to address the underlying structural issues and ensure timely access to quality dental care
In dentistry inequalities in the delivery of dental care services are greater than inequalities in the disease itself.
The government spends around NZ$16 billion annually on health and spends around a quarter of a billion dollars a year on dental care.
NZ’s dental care system demonstrates why we can’t rely on market forces to equitably distribute population health services. The cost of introducing universal coverage for dental care would be high but doesn't mean the idea should not be considered or variation of it.
Prevention - it isn't just about brushing teeth and water fluoridation. NZ needs to increase spend on preventative dental care to save on the high cost of dental interventions.
Cardiovascular disease, diabetes and obesity have many of the same causes as dental disease. Stricter limits on the marketing and sale of sugary drinks and lollies, better regulation of “hidden sugars” and continued efforts for tobacco control would have benefits beyond dental health.
Dentistry is poorly integrated with other areas of health care. Neither is it funded like other areas of health care.
Dental surgery is expensive just like any other form of surgery. Accessible dental care can’t happen without funding.
First steps towards the goal that all New Zealanders are able to access affordable dental care should be population-level prevention and ensuring that disadvantaged groups can access emergency dental care.
Central, Health. Dental Therapists: We Can Help Improve Access to Dental Care. 28 Jan. 2019, https://healthcentral.nz/dental-therapists-we-can-help-improve-access-to-dental-care.
Dental therapists are keen to see access to dental care improved for low income and older New Zealanders
The Association says that countries like Australia are “miles ahead” in terms of utilising the extended skills of dental and oral health therapists.
“We as a profession are ready to train further and ensure the most vulnerable receive equitable access. There is no shortage of dental and oral health therapy graduates in New Zealand and if we are to retain these graduates in our country then they need to be provided with the opportunity to extend their respective scopes. It’s a win-win for the professions and for the country.”
Norris, Pauline. ‘Gaps in the System’. Otago Daily Times Online News, 11 May 2020, https://www.odt.co.nz/lifestyle/magazine/gaps-system
Gaps in the system
There are some who can't afford to smile
Dental care for adults, however, has never really been part of this system. Dental care is provided free to children.
the "murder house" where a woman in a starched uniform drilled and filled our teeth without anaesthetic
In the latest, NZ Health Survey around half of the people surveyed (53%) said they only went to the dentist for problems or did not go at all. Maori, Pacific people, those on low incomes and people with mental health problems often miss out on dental care. People in rural areas without dentists also struggle. Late last year I was in a rural healthcare centre a couple of hours north of Gisborne when a young woman with severe dental pain turned up. She had managed to get an appointment with a dentist in Gisborne but had no transport so couldn’t get to the appointment
In a recent paper in the Journal of the Royal Society of New Zealand, John Broughton and his colleagues wrote about the dental health of Maori with mental health problems. They interviewed 32 people and asked about their oral health and its impact on their lives, using a standard questionnaire that has been used in many studies. People reported that their oral health was causing them psychological and physical pain and disability and affecting their social interactions.
…. Not surprisingly, getting all this necessary dental work done had a big impact on participants. They experienced lower levels of pain, discomfort, and disability, and it is likely that the treatment led to increased mental as well as physical health.
The study makes clear that there is a very large burden of serious untreated dental problems in the community, and suggests that people with mental health problems should be a priority group for receiving dental care. The authors point out that Maori ways of thinking about health stress the connections between physical, mental, family and spiritual health. In this case, it is really clear that poor physical health, like not having many (or any) teeth, or having pain or infection from bad teeth, are likely to lead to other health and social problems.
Jones, Nicholas. Give All Kiwis ‘comprehensive and Affordable’ Dental Care: New Zealand Medical Association . 6 Mar. 2019, https://healthcentral.nz/give-all-kiwis-comprehensive-and-affordable-dental-care-new-zealand-medical-association/.
About one in three New Zealanders have untreated tooth decay, the last comprehensive oral health survey in 2009 found. Almost half of adults had avoided routine dental treatment in the previous year, because of cost.
All New Zealanders should have access to a “comprehensive and affordable” dental service, the New Zealand Medical Association says.
“comprehensive dental service for all New Zealanders”
Association chairwoman Dr Kate Baddock said dental decay “remains the most prevalent chronic, yet reversible disease in New Zealand”.
Māori and Pasifika have worse oral health outcomes as well as those living in areas of higher socioeconomic deprivation – this is an equity issue that must be addressed
Baddock said bold action was needed to prevent dental problems, including fluoridation of drinking water, and cutting down on sugar in food and drink.
Any move to provide more subsidised or free dental care would carry a huge cost. Currently, about $198 million a year is spent on oral health services, with most covering universal services for children and teenagers.
Adults must pay the full cost, and bills can run into thousands of dollars.
Kiwis without enough money live in chronic pain that affects work, quality of life, and mental and wider health. Gum disease increases the risk of heart disease, and poor oral health increases the chances of bacterial infection in the bloodstream.
Slater, Caitlin. ‘Memories of Dental Nurses and the “Murder House”’. Stuff, 15 Feb. 2016, https://www.stuff.co.nz/national/health/76918041/memories-of-dental-nurses-and-the-murder-house.
During World War, I about 40 per cent of potential recruits were rejected because the poor state of their teeth meant they were not fit to serve.
Baker, Gabrielle. ‘Inequality in Dental Care Is a Treaty Issue’. The Spinoff, 7 Oct. 2019, https://thespinoff.co.nz/science/07-10-2019/inequality-in-dental-care-is-a-treaty-issue/.
once we turn 18 means that good oral health and regular dental visits are luxuries for many, requiring bravery and serious coin.
Oral health data also shows a picture of health sector failure, even when the service is “free”. For example, Māori and Pacific children under five are more likely than other children to have cavities (whether or not they live in areas with fluoridated water supply)
“Māori as Tiriti/Treaty partners have not been well served by the health and disability system. During the symposium oral health was described as a Cinderella policy area, in reference to it receiving less attention than it should from policymakers last national oral health policy, Good Oral Health For All, For Life, was released in 2006 and only one of the seven priority actions have been achieved. Meanwhile, the inequities in access to oral health services and in good oral health outcomes remain and there doesn’t appear to be any consequences (for the Ministry, DHBs or providers) for the lack of equitable progress.
Good oral health is central to our overall wellbeing (affecting our ability to do everything from smiling freely to chewing food easily) yet it is treated as a separate and siloed issue in terms of health funding. 77 per cent of general practice services are publicly funded compared to 24 per cent of dental services. This creates a very real barrier to access for people, partially explaining the steep costs we all experience as adults seeking dental care
Martin, Hannah. ‘“Appalling” Child Tooth Decay Rates in Northland and Auckland’. Stuff, 11 Apr. 2019, https://www.stuff.co.nz/national/health/111956057/appalling-child-tooth-decay-rates-in-northland-and-auckland.
Two-fifths of pre-schoolers in Northland and Auckland have tooth decay
But along the way, they found 40 per cent of the children had one or more decayed, missing or filled tooth surface in their primary (baby or milk) teeth
Aung and Tin-Tin said the "significant" and "surprising" association between tooth decay and injury admissions may be due to "common factors" relating to wider issues of social inequities – being from lower socioeconomic status, poor physical environments and large families
he data showed non-European children and those living in Northland – in more deprived areas or those without water fluoridation – had higher rates of tooth decay.
Of those surveyed, more than 64 per cent of Pacific and 59 per cent of Māori children had tooth decay.
It was "appalling" to see that two in five pre-school children had caries, Tin Tin told Stuff.
"This underscores the need for urgent public health actions to improve oral health and reduce inequalities in pre-school children," she said.
Rates of tooth decay in New Zealand far exceed rates overseas
Northland's lack of fluoridation in its water supply and New Zealand's "minimal" regulation around the availability and promotion of sugary foods and drinks also played a role, they said.
President of the New Zealand Dental Association, Bill O'Connor said Northland and Auckland's dental services were "overwhelmed".
The findings reinforced the association's position particularly around the role sugary drinks and water fluoridation played in oral health, he said
Both Northland and Auckland were experiencing shortages of oral health therapists, amid "huge demand"
Revive A Smile (nzdentalcharity.org)
Revive A Smile is a New Zealand based dental charity established in 2011 by Dr Assil Russeull and run by a team of dental health professionals from all over Aotearoa.
Revive a Smile aims to reduce oral health disparities experienced by disadvantaged and impoverished Kiwis.
The project works by providing much needed free dental treatment education and oral health products (such as health packs, including toothbrushes, floss and mouth wash.
Revive a Smile provides dental care and various members and groups of the community including homeless persons, victims of domestic violence, refugee migrants, low-income adults and the elderly. It aims to empower kiwis to take control of their oral health by treating toothache and developing personal skills, enabling people to become, healthy, contributing members of society.
Founded on Dr Russell’s philosophy that “caring creates change”
Revive a smile is a dental charity that is purely about caring indiscriminately without conditions.
Revive A Smile runs charity mobiles dental clinics and partner practices throughout New Zealand.
Are Supported by Southern Cross.
Random Input: Word In Class
Words given: Chicken, Wave and Bus
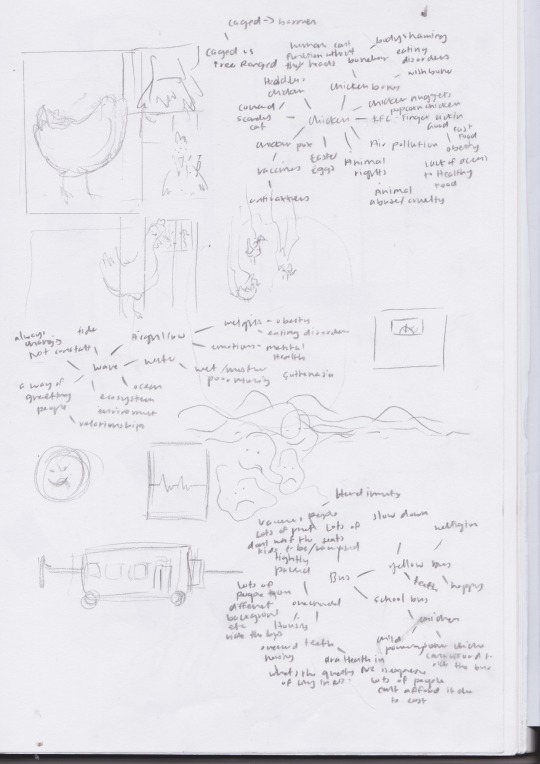
Daily Exercise: Random Input - Word and in response to reading: Hayden, Leonie. ‘Why Diversity Matters (and No One Should Need to Write This Headline in 2020)’. The Spinoff, 18 July 2020, https://thespinoff.co.nz/atea/18-07-2020/why-diversity-matters-no-one-should-need-to-write-this-headline-in-2020/.

For today’s poster I used the word I got from class: chicken for my poster. I wanted to try hand drawing it as opposed to doing it digitally as I really enjoyed it from Monday’s class the quick sketching of ideas. I played cut the pictures out then played around trying out different compositions before scanning it and editing it in photoshop. After doing the reading through my poster I wanted to show the key idea of “perspective being an asset”. In my poster I show two chicken one that is white the other that is of colour, the white chicken is able is free ranged and lives a life outside of a cage and is able to receive food. In comparison the chicken who is coloured is a chicken that is caged can only watch as the other eats.

Word List
Inequality
Bias
Difference
Discrimination
Disparity
Injustice
Unfairness
Contrast
Variation
Dentist
Tooth fairy
Murder house
Mad house
Murder
Assassination
Bloodshed
Crime
Destruction
Massacre
Butchery
Carnage
Teeth
Fang
Incisor
Molar
Premolar
Snag
Canine
Dent
Grind
Grinder
Mouth
Box
Cavity
Door
Entrance
Gate
Beak
Chops
Clam
Crevice
Funnel
Gob
Jaws
Trap
Portal
Bone
Cartilage
Abrasion
Plaque
Oral
Fracture
Extraction
Excision
Erosion
Dry mouth
Decay
Cusp
Crown - artificial
Cementum
Composite
Bicuspid
Waves of emotions



0 notes
Text
New Zealand food shouldn’t be defined by lolly mash-ups
OPINION: Search “New Zealand food” online and you’ll get a list of foods ranging from hangi to pavlova and anzacs to afghans. This is our food, but New Zealand is distracted by Pineapple Lumps, Jaffas, Moro Bars, Snifters, Sparkles, K-Bars, Buzz Bars and Pinky Bars.
from Ellie NZ Rss http://www.stuff.co.nz/life-style/food-wine/food-news/93869304/New-Zealand-food-shouldn-t-be-defined-by-lolly-mash-ups
from Ellie's Blog https://ellieplume83.wordpress.com/2017/06/22/new-zealand-food-shouldnt-be-defined-by-lolly-mash-ups/
0 notes