Photo


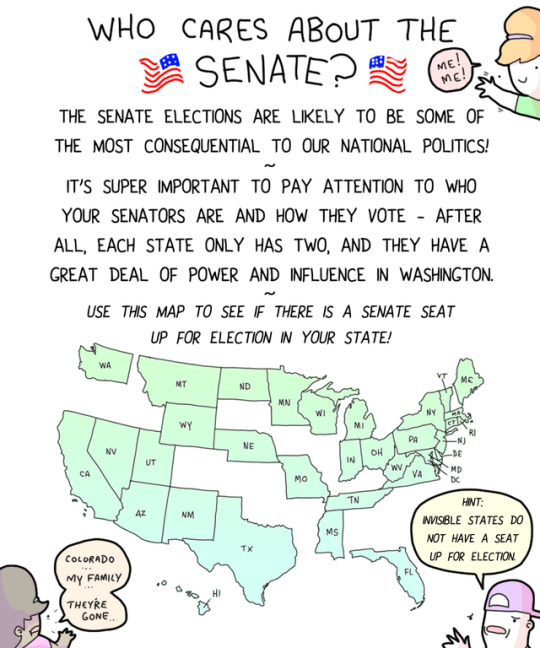


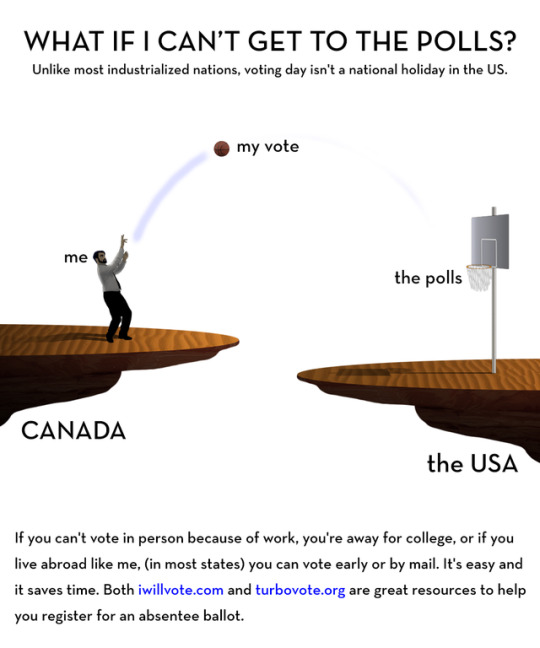

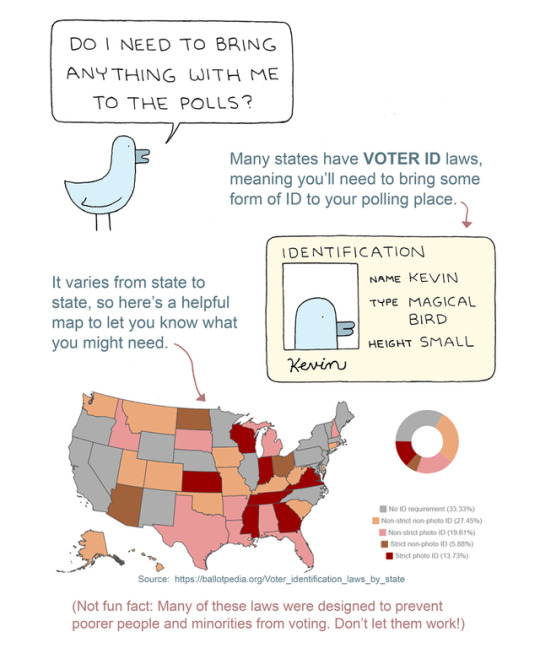

REPOST @TinySnekComics - you know what’s cool? VOTING THIS NOVEMBER!!! if you retweet anything today, make it is!!
19K notes
·
View notes
Photo








Blessing your day with some cute ass fluff dragons. Look at these lil sky puppies ❤😍😍😍
Ps i will be posting some actual DW stuff soon i promise
116K notes
·
View notes
Text
How to Support Someone With PTSD/C-PTSD
***This also applies to people who are supporting those diagnosed with DESNOS or trauma-based disorders***
Be patient. This is the first step to being a strong foundation for someone with this ailment; it can take days, months or years for the one you love to open up about what happened, express general emotions or even leave the home. When you show that you are patient with them in every way, you are showing them that you love them through thick and thin.
Educate yourself about PTSD/C-PTSD. This can be said about any learning disability, physical disability, mental health issue or neurodiverse diagnosis. Go to support groups, do your research and ask questions to specialists. Most importantly, ask the individual you are supporting if they are willing to explain how they are impacted on a daily basis. Please note that not every sufferer will want to elaborate further.
Do “normal”/conventional things with them. It sounds a little overdone, but people with this disorder have gone through anything but a stable surrounding, environment or event. Taking them to a movie, a walk in the park, out to the beach, for a picnic, to dinner or lunch, social event, etc. will show them that they are deserving of something more than the trauma they’ve been through.
Be accepting about unsaid/mixed feelings. Remember, it’s really challenging for a majority of people with this disorder to completely vocalize what they’ve been through. It takes a lot of time, specifically for people with C-PTSD, to express their feelings because sometimes they just can’t find the right words to explain it.
Learn to be an attentive listener. I’ll be making a post about this in the near future. Ask the right questions without accusing language such as, “WHY do you feel ______.” Instead try an alternative such as, “What about _____ is making you feel _______?”. Try to avoid saying “everything will be okay” or generally invalidating their feelings. When you invalidate someone’s feelings, they ultimately feel like they can’t trust you and that you don’t take their feelings seriously.
Minimize stress at home - aim to make the home as comfortable as possible. The last thing someone suffering with a trauma-based illness needs is instability within their home life. Give them time to relax and decompress from the daily stresses.
Create structure/routine in every day life. Someone who has been through trauma (typically) craves structure and consistency in order to remember that they have control over their lives. Having a set routine helps restore a sense of self-empowerment and security in the person dealing with their trauma-based struggles.
Encourage their strengths and talents. This will help the sufferer see through a different lense; a lense that shows them their ability, especially their capability of recovering and moving forward. The more someone grows from their talents, the closer they are to establishing and strengthening their sense of self again.
(Intimate relationships) Assure them that you are there for them and love them regardless of their illness. When you tell the person you love that their illness does not define them and that your love transcends beyond that, their trust will rebuild. Abandonment issues are rampant in those with trauma-based illnesses (although at the same time, sufferers get in modes of prolonged self-isolation). The more you assure them and show it through your actions, the more that trust rebuilds and they are less likely to become co-dependent.
Help them make new, happy memories. The last thing someone with PTSD/C-PTSD/DESNOS/etc. wants to think about is the past. Making new memories will help them move forward and start enjoying their new life.
Learn about the person’s triggers and stressors. Yes, they are different. In short, “a trigger is a symptomatic reaction from one of the five senses (sight, sound, touch, taste and smell) based only upon a direct connection to an actual traumatic event experienced,” while “a stressor is something that creates an increase in adrenaline that then triggers your internal stress response mechanism…Think iceberg of emotions: a buildup of negative emotion which peaks to a response, usually anger.“ (both courtesy of myPTSD.com). The more you become in tune with what is problematic to the person, the better you will get at navigating communication, help and support.
Be compassionate in how you approach things. It can be hard as the world tells us frequently to harden up; when you’re supporting someone who has suffered from trauma, yelling could be a stressor. Certain sayings can cause a downward spiral (especially if the perpetrator said those things verbatim, or the saying could be related to an event that the sufferer has gone through). Compassion is vital and lets the person know that they can trust you and continue to move forward.
Allow the person to talk about the past. Without saying, “Stop living in the past”. As mentioned in my previous post about what NOT to say to someone with PTSD/C-PTSD, that is an extremely invalidating and belittling thing to say to someone; sometimes the sufferer needs to talk about it in order to further their recovery.
Understand that trauma changes people. Once you can grasp that trauma really changes people and how they react to things, you can then begin to learn how to approach the person with a compassionate scope.
Know that identity confusion/issues are a common response with people who have trauma-based illnesses, especially in CSA survivors. It can take a lot of therapy and time for the dissociation and identity issues to subside; when you get more educated about trauma-specific illnesses, you’ll notice that this comes up a lot. Responding to someone who is confused about their identity, at that point in time, requires assurance. Telling them that you support their decisions and approaching it with openness will help clear their mind instead of making them feel like they’re going in a downward spiral.
Remain calm during emotional outbursts. This can be challenging because everyone has an innate fight-or-flight response. When you stay at the same tone of voice, give them some distance and say something such as, “Perhaps you need some time to decompress.” or “What can I do to help you?” the person will most likely start to gather themselves emotionally.
Apply self-care. In order to continue supporting someone with PTSD/C-PTSD, you need to care for yourself too, otherwise you’ll suffer from caregiver’s burnout. As they always say, “Take care of yourself or you can’t take care of anyone else.”
667 notes
·
View notes
Text
So true and depressing
“hi” almost every last message to all my crushes. They never replied.
40 notes
·
View notes
Photo





Friday, Cassini will dive into Saturn’s atmosphere and put an end to its nearly 20 year mission. Over those years we learned an incredible amount of information about Saturn, its rings, and its many moons. During the grand finale, Cassini will continue to send back information about Saturns atmosphere before burning up like a shooting star.
48K notes
·
View notes
Photo
Do this!




This Movie With Jeff Goldblum And Stanley Tucci Isn’t Real, But It Needs To Be
7K notes
·
View notes
Text
What’s Up for June 2017?
Have a planet party and compare Saturn and Jupiter! We’ll show you where and when to point your telescope or binoculars to see these planets and their largest moons.

Meet at midnight to have a planetary party when Jupiter and Saturn are visible at the same time!
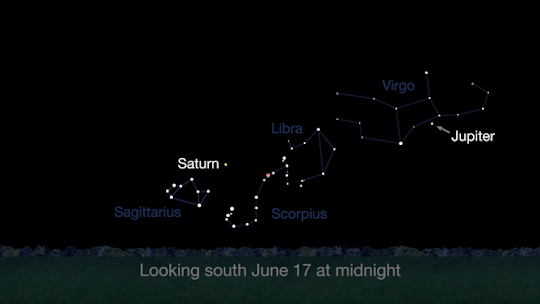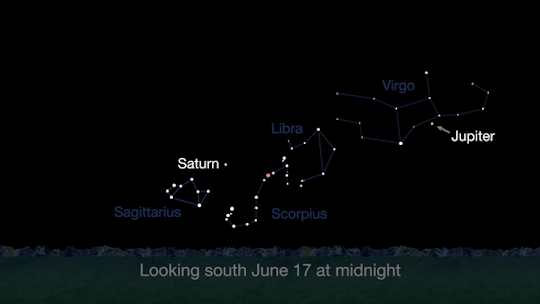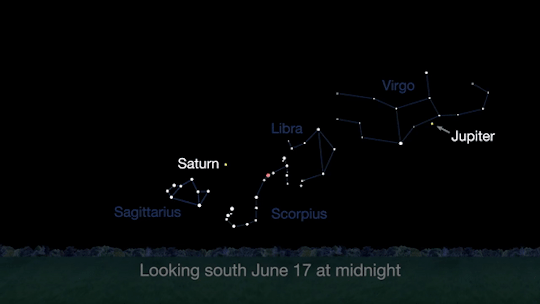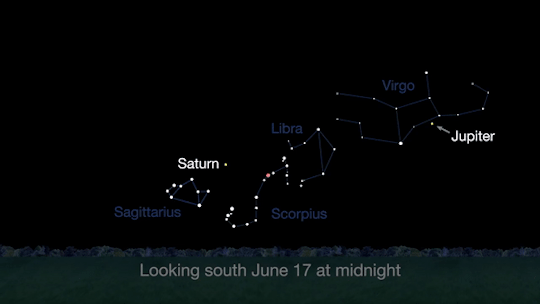
The best time will be after midnight on June 17. To see the best details, you’ll need a telescope.

Saturn will be at opposition on June 14, when Saturn, the Earth and the sun are in a straight line.
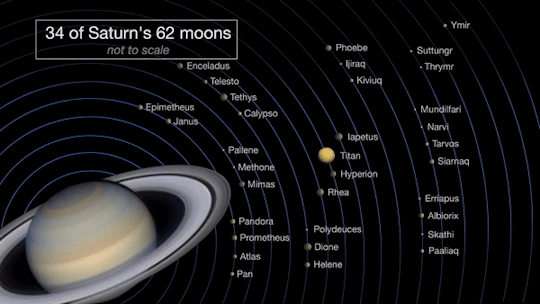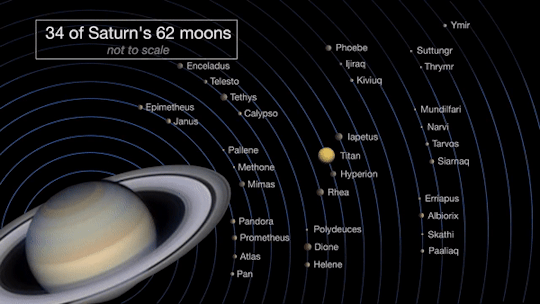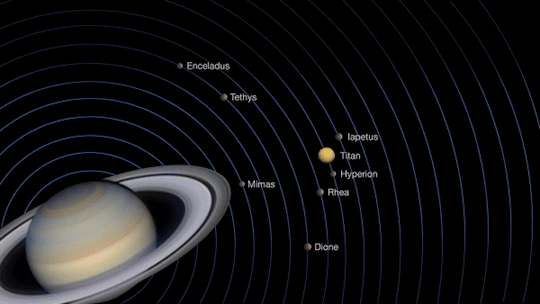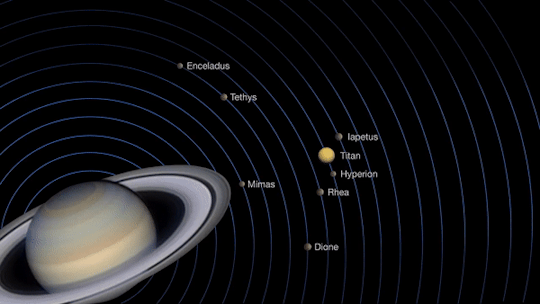
Opposition provides the best views of Saturn and several of its brightest moons. At the very least, you should be able to see Saturn’s moon Titan, which is larger and brighter than Earth’s moon.
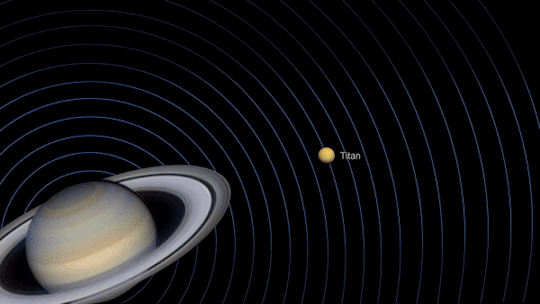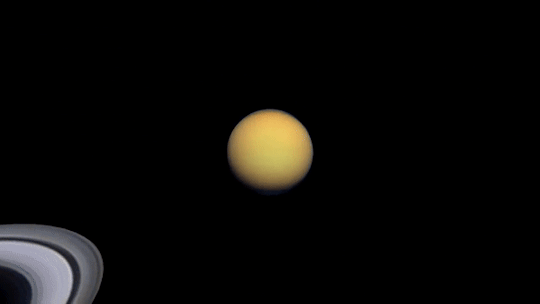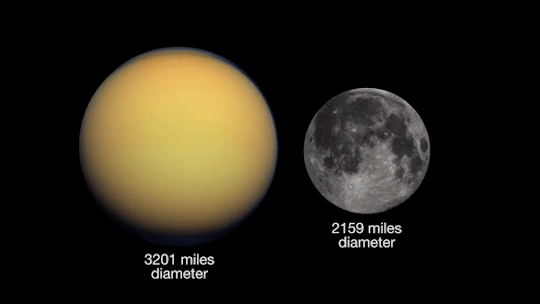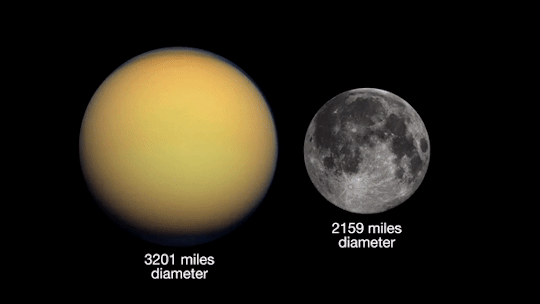
As mentioned earlier, you’ll be able to see Jupiter and Saturn in the night sky this month. Through a telescope, you’ll be able to see the cloud bands on both planets. Saturn’s cloud bands are fainter than those on Jupiter.

You’ll also have a great view of Saturn’s Cassini Division, discovered by astronomer Giovanni Cassini in 1675, namesake of our Cassini spacecraft.

Our Cassini spacecraft has been orbiting the planet since 2004 and is on a trajectory that will ultimately plunge it into Saturn’s atmosphere on September 15, 2017, bringing the mission to a close.

Our Juno spacecraft recently completed its sixth Jupiter flyby. Using only binoculars you can observe Jupiter’s 4 Galilean moons - Io, Callisto, Ganymede and Europa.

To learn about What’s Up in the skies for June 2017, watch the full video:
youtube
For more astronomy events, check out NASA’s Night Sky Network at https://nightsky.jpl.nasa.gov/.
Make sure to follow us on Tumblr for your regular dose of space: http://nasa.tumblr.com
2K notes
·
View notes
Video
youtube
As a neonatal intensive care nurse, Lauren Bloomstein had been taking care of other people’s babies for years. Finally, at 33, she was expecting one of her own. The prospect of becoming a mother made her giddy, her husband Larry recalled recently— “the happiest and most alive I’d ever seen her.”
Other than some nausea in her first trimester, the pregnancy went smoothly. Lauren was “tired in the beginning, achy in the end,” said Jackie Ennis, her best friend since high school, who talked to her at least once a day. “She gained what she’s supposed to. She looked great, she felt good, she worked as much as she could” — at least three 12-hour shifts a week until late into her ninth month. Larry, a doctor, helped monitor her blood pressure at home, and all was normal.
On her days off she got organized, picking out strollers and car seats, stocking up on diapers and onesies. After one last pre-baby vacation to the Caribbean, she and Larry went hunting for their forever home, settling on a brick colonial with black shutters and a big yard in Moorestown, N.J., not far from his new job as an orthopedic trauma surgeon in Camden. Lauren wanted the baby’s gender to be a surprise, so when she set up the nursery she left the walls unpainted — she figured she’d have plenty of time to choose colors later. Despite all she knew about what could go wrong, she seemed untroubled by the normal expectant-mom anxieties. Her only real worry was going into labor prematurely. “You have to stay in there at least until 32 weeks,” she would tell her belly. “I see how the babies do before 32. Just don’t come out too soon.”
When she reached 39 weeks and six days — Friday, Sept. 30, 2011 — Larry and Lauren drove to Monmouth Medical Center in Long Branch, the hospital where the two of them had met in 2004 and where she’d spent virtually her entire career. If anyone would watch out for her and her baby, Lauren figured, it would be the doctors and nurses she worked with on a daily basis. She was especially fond of her obstetrician/gynecologist, who had trained as a resident at Monmouth at the same time as Larry. Lauren wasn’t having contractions, but she and the ob/gyn agreed to schedule an induction of labor — he was on call that weekend and would be sure to handle the delivery himself.
Inductions often go slowly, and Lauren’s labor stretched well into the next day. Ennis talked to her on the phone several times: “She said she was feeling okay, she was just really uncomfortable.” At one point, Lauren was overcome by a sudden, sharp pain in her back near her kidneys or liver, but the nurses bumped up her epidural and the stabbing stopped.
Inductions have been associated with higher cesarean-section rates, but Lauren progressed well enough to deliver vaginally. On Saturday, Oct. 1, at 6:49 p.m., 23 hours after she checked into the hospital, Hailey Anne Bloomstein was born, weighing 5 pounds, 12 ounces. Larry and Lauren’s family had been camped out in the waiting room; now they swarmed into the delivery area to ooh and aah, marveling at how Lauren seemed to glow.
Larry floated around on his own cloud of euphoria, phone camera in hand. In one 35-second video, Lauren holds their daughter on her chest, stroking her cheek with a practiced touch. Hailey is bundled in hospital-issued pastels and flannel, unusually alert for a newborn; she studies her mother’s face as if trying to make sense of a mystery that will never be solved. The delivery room staff bustles in the background in the low-key way of people who believe everything has gone exactly as it’s supposed to.
Then Lauren looks directly at the camera, her eyes brimming.
Twenty hours later, she was dead.
Focus On Infants During Childbirth Leaves U.S. Moms In Danger
694 notes
·
View notes
Photo

Dog’s mom accidentally orders XS dogbed. Good Dog still grateful. (Source: http://ift.tt/2p7bDa3)
718 notes
·
View notes
Photo
Don't drink the kool-aid


Nearly 40 Years Later, Jonestown Offers A Lesson In Demagoguery
On Nov. 18, 1978, an itinerant preacher, faith healer and civil rights activist named the Rev. Jim Jones led more than 900 of his followers to kill themselves by drinking cyanide-laced Flavor Aid at their Jonestown settlement in the jungle of Guyana. Nearly 40 years later, questions still linger regarding the Jonestown massacre and the man who inspired it.
Journalist Jeff Guinn details how Jones captivated his followers in his new book, The Road to Jonestown. He calls Jones a “tremendous performer” who exhibited “the classic tendencies of the demagogue.”
Guinn says Jones, who founded Peoples Temple church, would take current events and exaggerate them to create a sense of fear and urgency. He drew his followers to Guyana by convincing them that America was facing imminent threats of martial law, concentration camps and nuclear war.
After claims of abuse in Jonestown surfaced, Rep. Leo Ryan, D-Calif., came to Guyana to investigate. A number of Jonestown residents sought to return to the U.S. with Ryan, but others opened fire on the delegation, killing the congressmen and four others. The mass suicide followed.
Guinn says the lessons of Jonestown still resonate today. “Jim Jones epitomizes the worst that can happen when we let one person dictate what we hear [and] what we believe,” he says. “We can only change that if we learn from the past and try to apply it to today.”
Photos: Jim Jones / victims of the Jonestown massacre
1K notes
·
View notes






















