#Disease Research
Text

MAGNA™: A Revolutionary New Technology for Studying Protein-Protein Interactions
#Protein-Protein Interactions (PPIs)#Drug Discovery#MAGNA™ Platform#Biological Research#Disease Research
0 notes
Text
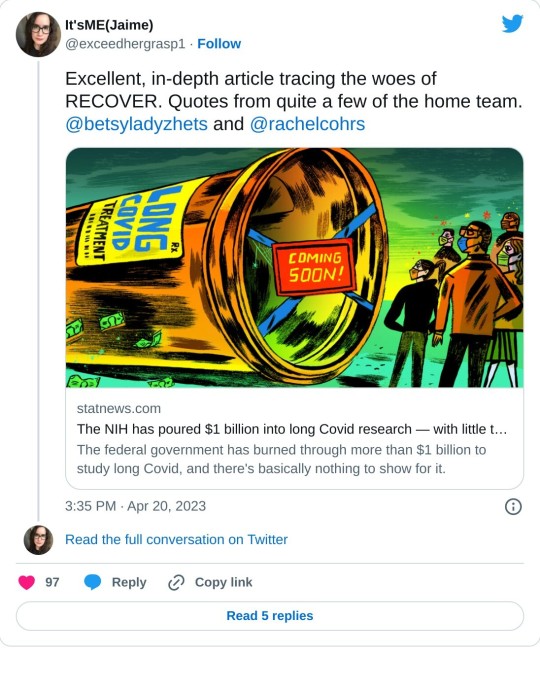
Take action on RECOVER and NIH below
#Long covid#Long haul covid#Long Covid Research#National Institute of Health#NIH#Disease Research#RECOVER INITIATIVE#RECOVER Program#RECOVER#Stat News#Jaimie Seltzer#ME Action Network#Public Health
0 notes
Text
American Airlines Skis for Cystic Fibrosis
American Airlines Skis for Cystic Fibrosis
American Airlines is donating $1.1 million to the Cystic Fibrosis Foundation, after their successful Celebrity Ski event early this month.
AA has had a long relationship with CFF, which works to raise awareness and fund research into the disease.
“For nearly four decades, we’ve gathered on the ski slopes with a group of generous team members, sponsors and supporters of the foundation to rally for…

View On WordPress
#american airlines#benefit event#cystic fibrosis#cystic fibrosis foundation#disease research#patrick feeley#ron defeo
1 note
·
View note
Text

Story from the Washington Post here, non-paywall version here.
Washington Post stop blocking linksharing and shit challenge.
"The young woman was catatonic, stuck at the nurses’ station — unmoving, unblinking and unknowing of where or who she was.
Her name was April Burrell.
Before she became a patient, April had been an outgoing, straight-A student majoring in accounting at the University of Maryland Eastern Shore. But after a traumatic event when she was 21, April suddenly developed psychosis and became lost in a constant state of visual and auditory hallucinations. The former high school valedictorian could no longer communicate, bathe or take care of herself.
April was diagnosed with a severe form of schizophrenia, an often devastating mental illness that affects approximately 1 percent of the global population and can drastically impair how patients behave and perceive reality.
“She was the first person I ever saw as a patient,” said Sander Markx, director of precision psychiatry at Columbia University, who was still a medical student in 2000 when he first encountered April. “She is, to this day, the sickest patient I’ve ever seen.” ...
It would be nearly two decades before their paths crossed again. But in 2018, another chance encounter led to several medical discoveries...
Markx and his colleagues discovered that although April’s illness was clinically indistinguishable from schizophrenia, she also had lupus, an underlying and treatable autoimmune condition that was attacking her brain.
After months of targeted treatments [for lupus] — and more than two decades trapped in her mind — April woke up.
The awakening of April — and the successful treatment of other people with similar conditions — now stand to transform care for some of psychiatry’s sickest patients, many of whom are languishing in mental institutions.
Researchers working with the New York state mental health-care system have identified about 200 patients with autoimmune diseases, some institutionalized for years, who may be helped by the discovery.
And scientists around the world, including Germany and Britain, are conducting similar research, finding that underlying autoimmune and inflammatory processes may be more common in patients with a variety of psychiatric syndromes than previously believed.
Although the current research probably will help only a small subset of patients, the impact of the work is already beginning to reshape the practice of psychiatry and the way many cases of mental illness are diagnosed and treated.
“These are the forgotten souls,” said Markx. “We’re not just improving the lives of these people, but we’re bringing them back from a place that I didn’t think they could come back from.” ...
Waking up after two decades
The medical team set to work counteracting April’s rampaging immune system and started April on an intensive immunotherapy treatment for neuropsychiatric lupus...
The regimen is grueling, requiring a month-long break between each of the six rounds to allow the immune system to recover. But April started showing signs of improvement almost immediately...
A joyful reunion
“I’ve always wanted my sister to get back to who she was,” Guy Burrell said.
In 2020, April was deemed mentally competent to discharge herself from the psychiatric hospital where she had lived for nearly two decades, and she moved to a rehabilitation center...
Because of visiting restrictions related to covid, the family’s face-to-face reunion with April was delayed until last year. April’s brother, sister-in-law and their kids were finally able to visit her at a rehabilitation center, and the occasion was tearful and joyous.
“When she came in there, you would’ve thought she was a brand-new person,” Guy Burrell said. “She knew all of us, remembered different stuff from back when she was a child.” ...
The family felt as if they’d witnessed a miracle.
“She was hugging me, she was holding my hand,” Guy Burrell said. “You might as well have thrown a parade because we were so happy, because we hadn’t seen her like that in, like, forever.”
“It was like she came home,” Markx said. “We never thought that was possible.”
...After April’s unexpected recovery, the medical team put out an alert to the hospital system to identify any patients with antibody markers for autoimmune disease. A few months later, Anca Askanase, a rheumatologist and director of the Columbia Lupus Center,who had been on April’s treatment team, approached Markx. “I think we found our girl,” she said.
Bringing back Devine
When Devine Cruz was 9, she began to hear voices. At first, the voices fought with one another. But as she grew older, the voices would talk about her, [and over the years, things got worse].
For more than a decade, the young woman moved in and out of hospitals for treatment. Her symptoms included visual and auditory hallucinations, as well as delusions that prevented her from living a normal life.
Devine was eventually diagnosed with schizoaffective disorder, which can result in symptoms of both schizophrenia and bipolar disorder. She also was diagnosed with intellectual disability.
She was on a laundry list of drugs — two antipsychotic medications, lithium, clonazepam, Ativan and benztropine — that came with a litany of side effects but didn’t resolve all her symptoms...
She also had lupus, which she had been diagnosed with when she was about 14, although doctors had never made a connection between the disease and her mental health...
Last August, the medical team prescribed monthly immunosuppressive infusions of corticosteroids and chemotherapy drugs, a regime similar to what April had been given a few years prior. By October, there were already dramatic signs of improvement.
“She was like ‘Yeah, I gotta go,’” Markx said. “‘Like, I’ve been missing out.’”
After several treatments, Devine began developing awareness that the voices in her head were different from real voices, a sign that she was reconnecting with reality. She finished her sixth and final round of infusions in January.
In March, she was well enough to meet with a reporter. “I feel like I’m already better,” Devine said during a conversation in Markx’s office at the New York State Psychiatric Institute, where she was treated. “I feel myself being a person that I was supposed to be my whole entire life.” ...
Her recovery is remarkable for several reasons, her doctors said. The voices and visions have stopped. And she no longer meets the diagnostic criteria for either schizoaffective disorder or intellectual disability, Markx said...
Today, Devine lives with her mother and is leading a more active and engaged life. She helps her mother cook, goes to the grocery store and navigates public transportation to keep her appointments. She is even babysitting her siblings’ young children — listening to music, taking them to the park or watching “Frozen 2” — responsibilities her family never would have entrusted her with before her recovery.
Expanding the search for more patients
While it is likely that only a subset of people diagnosed with schizophrenia and psychotic disorders have an underlying autoimmune condition, Markx and other doctors believe there are probably many more patients whose psychiatric conditions are caused or exacerbated by autoimmune issues...
The cases of April and Devine also helped inspire the development of the SNF Center for Precision Psychiatry and Mental Health at Columbia, which was named for the Stavros Niarchos Foundation, which awarded it a $75 million grant in April. The goal of the center is to develop new treatments based on specific genetic and autoimmune causes of psychiatric illness, said Joseph Gogos, co-director of the SNF Center.
Markx said he has begun care and treatment on about 40 patients since the SNF Center opened. The SNF Center is working with the New York State Office of Mental Health, which oversees one of the largest public mental health systems in America, to conduct whole genome sequencing and autoimmunity screening on inpatients at long-term facilities.
For “the most disabled, the sickest of the sick, even if we can help just a small fraction of them, by doing these detailed analyses, that’s worth something,” said Thomas Smith, chief medical officer for the New York State Office of Mental Health. “You’re helping save someone’s life, get them out of the hospital, have them live in the community, go home.”
Discussions are underway to extend the search to the 20,000 outpatients in the New York state system as well. Serious psychiatric disorders, like schizophrenia, are more likely to be undertreated in underprivileged groups. And autoimmune disorders like lupus disproportionately affect women and people of color with more severity.
Changing psychiatric care
How many people ultimately will be helped by the research remains a subject of debate in the scientific community. But the research has spurred excitement about the potential to better understand what is going on in the brain during serious mental illness...
Emerging research has implicated inflammation and immunological dysfunction as potential players in a variety of neuropsychiatric conditions, including schizophrenia, depression and autism.
“It opens new treatment possibilities to patients that used to be treated very differently,” said Ludger Tebartz van Elst, a professor of psychiatry and psychotherapy at University Medical Clinic Freiburg in Germany.
In one study, published last year in Molecular Psychiatry, Tebartz van Elst and his colleagues identified 91 psychiatric patients with suspected autoimmune diseases, and reported that immunotherapies benefited the majority of them.
Belinda Lennox, head of the psychiatry department at the University of Oxford, is enrolling patients in clinical trials to test the effectiveness of immunotherapy for autoimmune psychosis patients.
As a result of the research, screenings for immunological markers in psychotic patients are already routine in Germany, where psychiatrists regularly collect samples from cerebrospinal fluid.
Markx is also doing similar screening with his patients. He believes highly sensitive and inexpensive blood tests to detect different antibodies should become part of the standard screening protocol for psychosis.
Also on the horizon: more targeted immunotherapy rather than current “sledgehammer approaches” that suppress the immune system on a broad level, said George Yancopoulos, the co-founder and president of the pharmaceutical company Regeneron.
“I think we’re at the dawn of a new era. This is just the beginning,” said Yancopoulos."
-via The Washington Post, June 1, 2023
#mental illness#schizophrenia#schizoaffective#psychotic disorders#psychology#neurology#autoimmune#autoimmine disease#neuroscience#medical news#medical research#catatonia#immunotherapy#immune system#clinical trials#good news#hope
6K notes
·
View notes
Text

chronic wasting disease
#get it because chronic wasting disease is sometimes called zombie deer disease#I fell down a rabbit hole researching CWD for this#I didn’t really use it besides the decision to make the infected arm skin tight#geminitay#secret life#trafficblr#life series
418 notes
·
View notes
Text










sure sign that the brain worms are taking over ❤️
#i need research and funding put into whatever disease i have#jeffrey combs#cyclone 1987#doctor mordrid#the frighteners#trancers#had to include from beyond bc it’s pretty pink#but it’s not my favorite movie to say the least….#castle freak#love and a .45#reanimator#motivational growth
481 notes
·
View notes
Text

#pay attention#educate yourselves#educate yourself#knowledge is power#reeducate yourself#reeducate yourselves#think about it#think for yourselves#think for yourself#do your homework#do your research#do your own research#ask yourself questions#question everything#food#food supply chain#contaminated food#contaminated water#disease#history lesson#history#hidden history#government corruption#fda corruption#poisoning humanity#food poisoning
356 notes
·
View notes
Text
my pet peeve is those "historians thought they were very good friends" jokes, like obviously for sure there are homophobic historians, but the study of same-sex desire and relationships of the past is also quite complex and you can't often go and simply label people's relationships or identities of time gone by, and sometimes it's more complicated and elusive than "they were a couple" or even "they were in love"
#nor's rambles#being a bit of a queer theorist here#note also that historical research is interpreting source material and source material seldom is straightforward#different historians will likely come to different conclusions#i would also say!!! that i don't think a lot of people really know the history of labels and lgbtq+ knowledge#like lady gaga saying BORN THIS WAY can be liked all the way back to sexologists like havelock ellis saying that homosexuality is innate an#hence not a disease or a crime
555 notes
·
View notes
Text
Vaccines: The Unsung Heroes of Modern Medicine
Imagine a world where smallpox still reigned supreme, where polio paralyzed thousands annually, and where measles was a rite of passage, sometimes fatal. Yet, here we are, in a world where vaccines have valiantly vanquished these threats.
The paramountcy of vaccines in the annals of medical triumphs cannot be overstated. They are the quintessence of human ingenuity, a testament to our ability to combat nature's most insidious adversaries. Through the meticulous administration of vaccines, we have consigned diseases like smallpox to the historical archives and reduced the scourge of polio to a mere whisper in the annals of modern afflictions.
Statistically, the efficacy of vaccines is irrefutable. The World Health Organization estimates that vaccines prevent 2-3 million deaths annually. Consider the measles vaccine: a marvel of medical science that has reduced global measles deaths by 73% between 2000 and 2018. Similarly, the introduction of the polio vaccine has brought the incidence of polio down by 99%, from 350,000 cases in 1988 to just 33 reported cases in 2018.
Yet, amidst this triumph, there exists a cacophony of dissent. The sanctimonious detractors, draped in the garb of skepticism, pontificate about the perils of vaccination. They brandish anecdotes of adverse reactions as if they were incontrovertible evidence, ignoring the overwhelming preponderance of scientific data. Yes, vaccines, like all medical interventions, are not devoid of risks. However, the incidence of serious adverse reactions is exceedingly rare. The Centers for Disease Control and Prevention notes that severe allergic reactions occur in about 1 in a million doses of vaccines. To put this in perspective, the likelihood of being struck by lightning in any given year is approximately 1 in 500,000—twice as likely as experiencing a severe vaccine reaction.
The irony is palpable. The very individuals who eschew vaccines on the grounds of potential harm are often the beneficiaries of the herd immunity afforded by the vaccinated majority. Their sanctimony is not only misplaced but perilously undermines public health efforts. The resurgence of measles in recent years, driven by declining vaccination rates, is a stark reminder of the consequences of such misguided dogma.
In conclusion, vaccines are the silent sentinels, safeguarding humanity against the ravages of infectious diseases. Their unparalleled efficacy, coupled with an exceptionally low incidence of adverse reactions, renders the anti-vaccine rhetoric not only scientifically unfounded but also morally untenable. The sanctimonious naysayers, in their misguided zeal, imperil the very fabric of our collective health. Let us, therefore, celebrate vaccines for what they truly are: the unsung heroes of modern medicine.
#sanctimonious#science#disease#immunity#vaccine#bacteria#virus#pathogens#climate change#scientific-method#reality#facts#evidence#research#study#knowledge#wisdom#truth#honesty
94 notes
·
View notes
Text
A new study that analyzed the activity of more than 10,000 genes found that a drug being investigated to treat celiac disease prevented intestinal damage caused by gluten.
The research focused on the molecular mechanism of ZED1227, a treatment designed to block transglutaminase 2 (TTG), an enzyme that reacts with fragments of gluten. This reaction makes the fragments more recognizable to the cells that cause destruction of the nutrient-absorbing finger-like projections in the intestine of those who have celiac disease.
#interesting study and sounds promising!#that said im no scientist lol#but some interesting information im here#info#research#celiac#celiac disease#coeliac disease#autoimmune disease
105 notes
·
View notes
Link
nationalgeographic.com
Article:
Now we know how COVID attacks your heart Even patients with mild COVID symptoms could face a higher risk of developing heart disease and stroke
By Sanjay Mishra
Scientists have noticed that COVID-19 can trigger serious cardiovascular problems, especially among older people who have a buildup of fatty material in their blood vessels. But now a new study has revealed why and shown that SARS-CoV-2, the virus that causes COVID-19, directly infects the arteries of the heart.
The study also found that the virus can survive and grow inside the cells that form plaque—the buildup of fat-filled cells that narrow and stiffen the arteries leading to atherosclerosis. If the plaque breaks, it can block blood flow and cause a heart attack or a stroke. The SARS-CoV-2 infection makes the situation worse by inflaming the plaque and increasing the chance that it breaks free.
This can explain long-term cardiovascular effects seen in some, if not all, COVID-19 patients.
...
#covid#heart#heart disease#long covid#heart attack#cardiovascular#covid is vascular#article#research#national geographic
153 notes
·
View notes
Text
A–Aventio TGCF idea?? Wherein Civil God Veritas Ratio meets the infamous Ghost King Aventurine during his first mission cuz cuz like— The "live for me" paralels?!? The one who has all the luck partner as well?!? The villain who was actually not the Villain this whole time!?!? The loving humanity a little too much it causes the downfall of a god?!?!?!?
Rant AU in the tags proceed with caution
#Okay to put it into better words:#Veritas having once being a prince wanted to give everyone the prosperity of knowledge and became a civil god in the pursuit of it.#Sadly this backfires in people using that knowledge for their own greed and creating civil wars within it as well as unleashing far more#Destruction upon the land. And the other gods didn't help Veritas in stopping that bc see that's what happens when people overshare info!!#So the aftermath is just pure chaos plus banishment from being a civil god and thrown as this god of war and plague.#800 years passes and he is seen to just still be doing the same things but I a simple term. Teaching people to read and count.#Often times taking up mission and doing research on new pathogens to help cure the sick that can't afford and somehow during a reading#Lecture he gets ascended back to godhood and everyone is like ??? And even he is like ???#Well he doesn't care much about it and just continues to do what he's always done. Except that once in a while he has to take a detour#Mission to deal with ghosts and other malignant spirits. And upon one of those recurrences he finds himself aquaintanced with#The infamous Ghost King Aventurine. Who is mostly feared in heaven due to having beaten the strongest and wisest at their own games. Even#When the odds where fully against him.#As for Aventurine.#His life was harsh but as the prince had given a lot to the people#Not just education but also free them of diseases and sickness. One of which had struck his sister. He liked the prince and wanted to#Follow in giving and protecting the prosperity of the former kingdom. But the good things did not last and his family was struck in between#The many wars that took place. No matter how much refuge Kakavasha and his sister sought no place was ever#Safe enough for them.#He watched the entire world go up in flames yet somehow he could hate the prince-god for it. But rather the people who had started to#Create weapons in his name. The rest of his years he spent it as a warrior slave and then when death reached him he couldn't even go to#The afterlife since he still held so much vigor and wanted revenge to all the people who had turned his land into ashes and his family#Into bones. That is why he became a mourning ghost.#(I didn't want the kakavasha story to be so centered on ratio like it is in tgcf. Because I think it will be fun for the two of them to#Not recognize each other at first after 800 years and then when they do. Rather when aven does he's full on: oh shit it's the cute prince—#As for who was the cause of the upheaval in the kingdom and the maker of the weapons. Idk I was debating there being more than just one#Antagonist to have pulled their strings in verita's kingdom as well as be the reason Aven's sister died. So he's more revenge seeking for t#And the genius society as civil gods just spoke to me it for so perfectly. Ling wen as Ruan mei? Yeah exactly.#ratiorine#Aventio#Dr ratio
28 notes
·
View notes
Note
What do you think Odile does for a living? She feels teacher like to me. What do you think she would do post canon?
HMMMM THIS IS GOOD QUESTION…
ive seen a lot of people hc her as a teacher / professor so i!! think that suits her pretty well. specifically as someone who studies + specializes in different types of craft (that would be why shes so proficient in multiple craft spells. also how she was able to figure out the loops stuff, AND to find something that could prevent siffrin from looping back).
post canon i am not sure… i am always torn between how the party would handle things post canon. obviously they would keep travelling for a bit, odile alongside her family without the stress of. constant sadness encounters + a king to kill lol. i think maybe she would get to take her time, reeaally get to know vauguardian culture when not within. a crisis. as was her original intention.
eventually. EVENTUALLY. when the family settles down somewhere (i am a “they all get a big house together” believer lol) she would get back into craft stuff. maybe go back into teaching too—surely people would be eager to hire a saviour. especially though i think it would be neat of her to try looking into wish craft etc, as a long forgotten form of craft. to satisfy her own curiosity, for siffrins sake, or just as a way of preserving the countries culture in whatever ways possible.
#asks#ive never gotten to talk about this before#and its a little unrelated to the odile thoughts so im putting it in the tags#but. surely surely. there must be some group out there dedicated to looking into this. suddenly lost island#no one remembers the country ofc. i bet its hard to even think about. probably difficult to dedicate an entire project to#but you also have to imagine. the day the island disappeared. the effect without anyone realizing why#people from the island. vacationers or visiting family etc. going through some sudden spell of amnesia all at once#and their loved ones + family being equally confused#also the fact that? given bambouches (probable) proximity to the island. that many of these cases wouldve popped up there#what did people think was going on. at the time. did they assume it was a disease?? a curse?#and then forget about the entire ordeal a week later#anyway point is. someone mustve found that suspicious. theres gotta be at least one person#which to me means i find it very likely there could be research gone into it. esp esp since the party members knew about. Some island that#isnt there#anyway anyways im rambling way too much#i think odile should look into wish craft. i think siffrin would appreciate it#if not because. it was a piece of him that was Important#but also to impart the actual Dangers of it to. others#am i making sense i dont know#isat spoilers#anyways oops thats not about odile anymore#lol
26 notes
·
View notes
Text
"For the first time, genetically modified pig kidneys provided “life-sustaining kidney function” during the course of a planned seven-day clinical study—a first step in addressing the critical crisis worldwide of kidney donor organ shortage.
The University of Alabama’s pre-clinical human study at Birmingham also advances the science and promise of xenotransplantation as a therapy to potentially cure end-stage kidney disease—just as a human-to-human transplants can.
“It has been truly extraordinary to see the first-ever preclinical demonstration that appropriately modified pig kidneys can provide normal, life-sustaining kidney function in a human safely and be achieved using a standard immunosuppression regimen,” said UAB transplant surgeon scientist Jayme Locke, M.D., director of UAB’s Comprehensive Transplant Institute and lead author of the paper...
The peer-reviewed findings published last month in JAMA Surgery describes the pioneering pre-clinical human research performed on a recipient experiencing brain death...
The pre-clinical human brain death model developed at UAB can evaluate the safety and feasibility of pig-to-human kidney xenografts, or transplants, without risk to a living human. It is named for transplant pioneer Jim Parsons, an organ donor whose family generously donated his body to advance xenotransplant kidney research, like the latest patient did.
A Critical Need
Kidney disease kills more people each year than breast or prostate cancer, while more than 90,000 people are on the transplant waiting list. More than 800,000 Americans are living with kidney failure and 240 Americans on dialysis die every day. The wait for a deceased donor kidney can be as long as five to 10 years, and almost 5,000 people per year die waiting for a kidney transplant.
Groundbreaking Study Details
The 52-year-old study subject for this research lived with hypertension and stage 2 chronic kidney disease, which affects more than one in seven U.S. adults, or an estimated 37 million Americans. As part of this study, the subject had both of his native kidneys removed and dialysis stopped, followed by a crossmatch-compatible xenotransplant with two 10 gene-edited pig kidneys, or UKidney.
The transplanted pig kidneys made urine within four minutes of re-perfusion and produced more than 37 liters of urine in the first 24 hours. The pig kidneys continued to function as they would in a living human for the entirety of the seven-day study. Also, the kidneys were still viable at the time the study was concluded.
“In the first 24 hours these kidneys made over 37 liters of urine,” said Dr. Locke. “It was really a remarkable thing to see.” ...
Gene editing in pigs to reduce immune rejection has made organ transplants from pigs to humans possible. The natural lifespan of a pig is 30 years, they are easily bred, and they have organs of similar size to humans. Genetically modified pig kidneys have been extensively tested in non-human primates, and the addition of UAB’s preclinical human research model—the Parsons Model—now provides important information about the safety and efficacy of kidneys in human transplant recipients."
-via Good News Network, September 17, 2023
#organ donation#organ donor#organ transplant#medical news#medical research#pigs#kidney transplant#kidney diseases#dialysis#good news#hope#hope posting#human biology
566 notes
·
View notes
Text

system collapse
#i have a rare disease where every time art drone is mentioned i picture a longer furby. incurable#the murderbot diaries#system collapse#system collapse spoilers#asshole research transport#perihelion#my art
103 notes
·
View notes
Text
will solace would've been a fan of valdevia
#he would research what parts of dna have to be affected for diseases to happen#and look through every ancient text/medical documents there are at camp to see if something ever happened#maybe he would think of the ways he can cure it#or make people fall sick#pjo#percy jackson and the olympians#will solace#heroes of olympus#hoo#frog speaks#will solace is a bio freak
25 notes
·
View notes