#nurse care manager
Text
Sell Benefits Not Features to Wealth Managers
Sell Benefits, not Features to Wealth Managers to Grow your Bottom Line
Selling benefits, not features, to wealth managers is a key to great marketing. Do you know how you do that?
When you market Geriatric care management, what makes the sale is ” What’s in it for me, the 3rd party?”. “Benefits answer that question for your targets.
Learn how to make an excellent marketing presentation that…

View On WordPress
#aging family#aging life care manager#aging parent care#aging parent crisis#Benefits#benefits of ALCA#Benefits Of Geriatric Care Managers#benefits to 3rd parties#black american geriatric care managers#black american social workers#Black Nurse Entrepreneurs#Black RN&039;s#Black travel nurses#care manager#case manager#dysfunctional aging family#Entitled Family#geriatric care manager#marketing to wealth manager#Narcissism#Narcissistic Personality#nurse advocate#nurse care manager#reaching top 10% elder#Wealth Management Banks#wealthy clients
0 notes
Note
Hey so your post about pain management as a bedside nurse is so important to my own nursing practice that I've considered printing it out so I can have it to hand all the time. So thanks for that. Also, how do you deal with assignments that are busy enough that pain management is harder than it should be? I'm coming up on two years as a nurse and I feel like I take it personally when I am too busy to adequately manage my patients pain. I'm also coming from a newly unionized hospital where the ratios are still horrendous (I do 1:10 on med surg) and I'm hoping once we can enforce our staffing grids it'll be better but idk I'm burning out and I love my job so much and I really respect your nursing philosophy? I guess. Sorry for the word vomit it's been a crazy shift.
I've been trying to think of how to answer this since I got it. It's just such a horrendous ratio. With ten patients a shift, that's like six minutes an hour for each in a fantasy world where there's no charting and everything is exactly where you need it to be. I feel like I don't have great insight into this because the most med surg patients I've had assigned is five. Ten patients to one nurse is just a raw deal for everyone. Like christ no wonder you feel like you're burning out! I'll give you what thoughts I have and hopefully other people can chime in if they have suggestions. But that's such a hard patient load.
When I've been super swamped, I've found that's when being really explicit about your thinking with the patient helps. Like if I have to dash into a room and then dash back out, I'll make sure the board is updated with the next medication time and that the patient knows when the medication is going to kick in. I'll also provide call light parameters. I have a lot of success telling people, "the med should be doing something by 5:30. If I haven't checked in with you by then, and the pain is unchanged or barely changed, hit your call light and we'll try the next step. Also hit your call light if you feel any sudden change, like now you're nauseated or you have a headache or the type of pain changes or something just feels very wrong. Is there anything you need before I step out of the room?"
I like to be explicit about when to call me because I think there's two directions call light usage can go wrong: someone calls all the time, or someone never calls. With someone who calls all the time, I find that telling them when I'll be back and that I want them to call me if I'm not takes away some of that anxiety that can causes some people to call frequently. Often those patients are afraid that if they aren't on the call light, they're gonna get ignored.
For the other type of patient, the one that doesn't call, I want to make explicit that it's GOOD AND NORMAL TO CALL YOUR NURSE WHEN YOU HAVE SYMPTOMS. We've all had that patient at the end of shift who goes, "btw the gnawing pain in my leg is now a 10/10" and you're like "what gnawing pain sir?? you've literally never mentioned it before now?? I don't have any meds for that lemme page super quick????" These patients can get into pain crises easily because they don't ask for help until something is unbearable. In addition to pain crisis bad, it takes a lot more time to deal with something unbearable than it does to deal with something uncomfortable.
On that note, are you spending your very limited time efficiently? To me, that actually means spend more time talking with patients, at least up front. Manage expectations, make sure people know what to expect. Having conversations with patients that are like, "You just had surgery, it's not gonna happen that we get you completely painless. We want to get you to a manageable pain level that allows you to do whatever it is you most want to do this shift." (For me on nights, that's usually sleeping at least a little, but sometimes the realistic goal you make together is that you will feel at some point better than you feel right now.) "You have this medication scheduled, and you have this one available every X hours when your pain is severe. Is there anything you know that helps you deal with pain?"
Also establish if patients want to be woken up for certain prn medications or if they're sleeping, to let them sleep. With some patients, I will advise them to get woken up for pain medication because I know that they're going to need consistent control to avoid a crisis. (Crises take so much time!)
When I'm crunched for time, I'm fond of bringing in an ice pack and being like "if it works, great, if it doesn't, just take it off, either way here it is." Sometimes I'll do the same with a warm blanket. If I know my patient needs to take pills, I'll bring a cup of water with me into the room. If there's a basic prn like melatonin or tylenol that I think they might want, I'll pull them in advance. If the patient doesn't want them, I return them next time I'm in the med room. (Obviously, don't do this with controlled substances. It's super easy to forget to return them, and not returning opioids is one of those whoopsies people get fired over.)
Decision making takes time. Walking to go get stuff takes time. I want to save the time it takes to assess if the patient needs those things and then walk off to fetch them by just having the things already. If your tightest resource is time, be liberal with resources you can spare. If you're stuck with a patient, do you have anyone you can delegate a prn med pass to? Do you know how to do the absolute minimum charting you need to? Do you have flushes and alcohol wipes and whatever other most common things you need? And since you can't hoard time, if you've got some to spare, ask yourself if there is anything you can do now that will save you time later. If you have five free minutes now and an incontinent patient, getting them up to the bathroom now can save you from taking the time for incontinence care and a bed change later on when they've also sundowned and decide they hate everything but most of all you.
So much of this answer I realize is investing as much time upfront as you can, which I realize is so hard when you are so busy. It sucks immensely that prepping takes much less time than not being prepared does when you don't always have time to prep. Plus when you invest that time to pain plan with patients and do small preventative interventions, I think it also provides some psychological comfort that helps with pain. You're letting them know you're invested and you care and you have a plan, even if you don't have all the time you'd like. That can mean better pain control, which can mean needing to spend less time in that room overall, meaning you can save six whole minutes at some point and maybe even, if we're feeling crazy, get a chance to indulge in that greatest of indulgences: just a real leisurely on-shift piss.
#nursing tag#i hope this helps at all i know how much it sucks to end a shift like 'cool. i didn't help my patients. feel great about that.'#it sucks when you don't have enough time to take care of people because you have too many people to take care of#anyway also thank you re: pain post compliment. and also thank you re: getting to talk about pain mgmt again#marge simpson holding potato voice: i just think [nursing process and symptom management] is neat!
145 notes
·
View notes
Text
i'm thinking of opening comms again soon (maybe this weekend) now things have settled down for me, but i'd like to lighten my workload stress, so! i'm figuring out a wait-list format and extending my turnaround time :>
#barks#also may lower prices again slightly as i have some annoying bills coming up#and usually i hold myself to finishing it within the week of payment but would just extend that to like. two weeks lmao#i'm also applying for a course in animal care/vet nurse training so having better managed work routines will be gooooood
21 notes
·
View notes
Text
.
#just saw a post that was like 'if you have religious or moral objections that stop you from providing certain types of medical care maybe#you shouldn't work in healthcare' (paraphrased) and...#what a way to look at the world tbh#like. they're talking about me i think - i am a conscientious objector when it comes to euthanasia#(which granted has come up exactly twice and both cases in a theoretical capacity only this is not a frequent request to me)#and... i am also a good doctor#last week i told someone that her weight doesn't matter to her health with receipts to prove it and she cried#no one had ever told her that before#and that was something that came from me specifically. that was something i would not trust all of the GPs in my practice - a practice of#excellent and compassionate GPs! - to say#i am verifiably doing good in my job that is coming from specifically who i am as a person#i cannot put that down when it comes to issues i care deeply about#fundamentally the fact that i cannot put it down is what makes me a good doctor#i think that's what i'm trying to get at#the reason that i do well by my patients is that i practice out of my values and my ethics#if i did not stand on that core i would not stand at all#so you can't have it both ways. you can't have engaged and active and compassionate healthcare providers without sometimes those engaged an#active providers having things they do not feel comfortable doing#and it is to everyone's service if they are up front about it and do not try to hide (i am suspicious of people who try to hide this)#i am literally figuring this all out as i type hence the v long tag ramble and also being nowhere near the post that started this train#(honestly in med school we talked so much about ethics as like. abortion! euthanasia! trans rights! and the ethics in practice is the littl#things. do you apologise when you mess up. how do you manage a consult with your patient with paranoid dementia and her child in the same#room at one time - or one by one bc that's fraught too. (that one's on top i had one of those today.) how do you act with grace when#you're a bit stressed and your patient is a bit stressed and the nurse wants to add five more things to your book. the day to day ethics is#SUCH a bigger thing when you come to actual practice.)#this is obviously entirely about me and leans on the fact that i largely do think i am doing a good job i am really feeling my own way#to a Thought. but i think to a certain extent it is generalisable
9 notes
·
View notes
Text
— 15 Questions for 15 or maybe 5 or 6 Friends —
I was tagged by @figkeele last week and tonight I don't feel like going to sleep yet (which is a GREAT idea) and haven't done one of these in a while, so here we go. Thank you!
Are you named after anyone? My dad.
When was the last time you cried? On Tuesday while reading Archangel's Lineage (Guild Hunter #16) by Nalini Singh. No worries, everything ends well, but one scene made me cry like rain. In felt very cathartic, though. A girl needs a good cry once in a while.
Do you have kids? No.
What sports do you play/have you played? None. Too sick for it.
Do you use sarcasm? Nah, never. Why do you ask? /s
What’s the first thing you notice about people? Voice/tone or IDK, vibe? *shrug*
What’s your eye color? Green.
Scary movies or happy endings? Happy endings. Life's hard enough, thank you very much.
Any talents? Writing? (Haven't written in... too long, though). Singing? (Same.)
Where were you born? To quote the mayor: in the most beautiful city in the word. :P
What are your hobbies? Reading, watching TV, crocheting.
Do you have any pets? Sadly, not currently.
How tall are you? Super tall, a whole meter and a half. :P
Favorite subject in school? Geography.
Dream job? I sort of have it? I've been completely quiet about it as not to jinx it, but last year I began work rehabilitation at a primary school with part-time teaching individual students and part-time doing admin and it turned into tentative government-subsidised employment this year... I like it a lot and I'm hoping really hard that becomes something more permanent. Cross your fingers, please! And don't envy me, it's still hard AF (health-wise) but if I have to work to live I'd at least like to do something I like, such as this.
Tagging (no pressure if you don't wanna do it): @wellwhataboutme, @eveningspirit, @stargazerdaisy, @jadedbirch, @abedsmessedupmeta, @zoi-no-miko and anyone else who wants to do it.
#tag meme#now you know why i've been more on down low on tumblr for the past year or so#too tired from work#(and also my mother's health got bad last year & had to take care of her even more but i managed to find her a place in a good nursing home#personal#about me
6 notes
·
View notes
Text

Accepted a job offer today. I am going to be the Quality Assurance RN for a local nursing home. They are about 6 months into a major revamp and overhaul. I had a long interview with the DON and I really like her vibe. She genuinely seems invested in improving the facility, and I think I will be helpful in that goal.
So I have about a week left of enjoying not working. But I will be happy to be back to work before I would have had to dip into savings to pay the mortgage.
#ha-hh#rn#new job#quality assurance#risk management#quality improvement#post-acute care#nurse#nursing
9 notes
·
View notes
Text
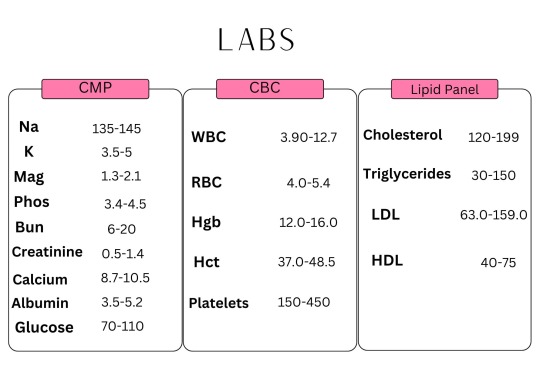
#icunurse#nursing school#nursing#etsy#icucare#hospital#icu#health and wellness#healthcare#diagnosis#diagnostic management software#medblr#patientcare#patientsafety#medical care#bloodwork#labs#note cards#reference#nursing studyblr#nursing student
4 notes
·
View notes
Text
The Role of Home Nursing in Chronic Disease Management

Chronic diseases are long-term health conditions that cannot be cured but can be managed with proper care and treatment. According to the World Health Organization (WHO), chronic diseases are the leading cause of death and disability globally, accounting for over 70% of all deaths worldwide. These diseases include cardiovascular disease, diabetes, cancer, and respiratory conditions such as asthma and chronic obstructive pulmonary disease (COPD).
Home nursing is a form of medical care provided in the patient's home rather than in a hospital or nursing home. Home nursing can be an effective option for patients with chronic diseases, as it allows them to receive the care they need in the comfort and convenience of their own homes.
The Benefits of Home Nursing for Chronic Disease Management
One of the main benefits of home nursing for patients with chronic diseases is the comfort and convenience of receiving care in their homes. For many patients, the familiarity and comfort of their own surroundings can be a significant source of comfort and stress relief.
Home nursing also allows personalized care based on the patient's specific needs. A dedicated team of healthcare professionals can provide care tailored to the patient's condition and lifestyle rather than a one-size-fits-all approach. This can be especially beneficial for patients with complex or multiple chronic conditions.
Another advantage of home nursing for patients with chronic diseases is the reduced risk of hospitalization and readmission. By providing care at home, patients can avoid the stress and potential complications of a hospital stay and receive the support they need to manage their condition at home. This can also help reduce healthcare costs, as hospital stays can be costly and strain the healthcare system.
Improved quality of life is another benefit of home nursing for patients with chronic diseases. By receiving care in the comfort of their own home, patients can maintain a sense of independence and continue with their daily routines and activities. This can help to reduce feelings of isolation and improve overall well-being.
Types of Chronic Diseases That Benefit from Home Nursing
Home nursing can be beneficial for patients with a wide range of chronic diseases, including:
Chronic respiratory conditions such as COPD and asthma: Home nursing can help patients with respiratory conditions to manage their symptoms and prevent exacerbations, which can lead to hospitalization. Services may include medication management, oxygen therapy, and education on self-management strategies.
Cardiovascular diseases such as hypertension and heart failure: Home nursing can help patients with cardiovascular conditions to manage their blood pressure, monitor their heart function, and make lifestyle changes to improve their health. Services may include medication management, monitoring of vital signs, and support for lifestyle changes.
Diabetes: Home nursing can help patients with diabetes to manage their blood sugar levels, prevent complications, and maintain a healthy lifestyle. Services may include medication management, insulin therapy, education on self-management strategies, and support for lifestyle changes.
Cancer: Home nursing can help patients with cancer to manage their symptoms and side effects and provide support during treatment. Services may include medication management, wound care, and education on self-management strategies.
Dementia and other neurological conditions: Home nursing can help patients with dementia and other neurological conditions maintain their independence and quality of life and support their loved ones. Services may include medication management, assistance with daily activities, and support for caregivers.
Home Nursing Services for Chronic Disease Management
Home nursing agencies typically offer a wide range of services to help patients with chronic diseases manage their condition and improve their quality of life. Some of the services that may be offered include:
Medication management: Home nurses can help patients to manage their medications, including ensuring that they are taking their medications as prescribed and keeping track of refill schedules.
Monitoring and management of vital signs: Home nurses can monitor the patient's vital signs (such as blood pressure, heart rate, and oxygen levels) and make any necessary adjustments to the patient's care plan.
Education and support for self-management of the disease: Home nurses can provide education and support to help patients learn how to manage their condition independently, including strategies for self-monitoring and self-care.
Coordination with the patient's healthcare team: Home nurses can work closely with the patient's primary care provider and other healthcare team members to ensure that the patient is receiving the best possible care.
Assistance with daily activities and self-care: Home nurses can provide assistance with activities of daily living (such as bathing, dressing, and grooming) and help patients to maintain their independence.
Challenges and Considerations in Home Nursing for Chronic Disease Management
While home nursing can be a valuable resource for patients with chronic diseases, there are also challenges and considerations to keep in mind. Some of the challenges and considerations include the following:
The importance of having a dedicated and reliable home nursing team: It is important to ensure that the home nursing agency provides a team of dedicated and reliable professionals who can meet the patient's needs.
Ensuring the safety and cleanliness of the home environment: It is important to ensure that the home environment is safe and clean and to make any necessary modifications to accommodate the patient's needs.
Coping with the emotional and psychological aspects of chronic illness: Chronic illness can be emotionally and psychologically challenging for the patient and their loved ones.
Financial considerations and potential cost savings: Home nursing can be a more cost-effective option for patients with chronic diseases, especially if it helps to prevent hospitalization and readmission. However, it is important to consider the financial implications and research potential funding sources (such as insurance coverage or grants) to help cover home nursing costs.
In conclusion, elderly care services such as home nursing and home care can be vital in managing chronic diseases. By providing care in the comfort and convenience of the patient's own home, home nursing services can help elderly patients to maintain their independence, improve their quality of life, and reduce the risk of hospitalization and readmission.
It is important to choose the right home nursing agency to meet the patient's needs and to consider the challenges and considerations involved in home nursing for chronic disease management. Home care services, such as assistance with daily activities and companionship, can also be an important part of the care plan for elderly patients with chronic diseases.
If you or a loved one is living with a chronic disease, consider the benefits of home nursing and home care services and talk to your healthcare provider about whether they might be a good option.
2 notes
·
View notes
Text
Hospice Los Angeles | All Treatment Objectives Are Met

Our skilled team of hospice Los Angeles counselors, nurses, and social workers collaborates with your physicians to ensure you receive the therapy and care you need. That is something we have seen make a huge impact on our patient's health. Having a sick loved one may be exhausting, but we are here to help ease your mind by ensuring that all of their doctors are in constant contact with one another. The goal of hospice and palliative care is to alleviate suffering and allow the patient or their loved ones to concentrate on resting and recuperating. Here we want to ensure you get exactly what you need. Hospice is often avoided because individuals feel it represents "giving up" on themselves or their loved ones. The true purpose of hospice service is to provide a calm and soothing environment for patients and their loved ones. The focus is on bettering one's standard of living.
#Hospice#Dignity#Hospice Care Services#Medical Care#Home Health#Care#Life#Physical#Emotional#Patients#Compassion#Spiritual#Clinicians#Doctors#Counsellors#Nurses#Medical#Los Angeles#Physical Therapy#Pain Management#Palliative Care#Medical Care Providers#Palliative#Retirement Home#Best Housing Options#Hospice Near Me
3 notes
·
View notes
Text
7 Tips For Feuding Midlife Siblings on Mother's Day
Celebrate Mother’s Day without the drama. Dote on Mom, but Ditch the Daggers.
Celebrations on Mother’s Day, this coming Sunday, or any holiday can be a nightmare for adult siblings in a dysfunctional family. They have to show up, yet they prepare with the daggers – either wielded by them or a fellow sibling.
Here are 7 tips for adult siblings to follow on holidays like Mother’s Day this…
View On WordPress
#adult sibling#adult sibling conflict#adult sibling estrangement#aging dysfunctional family#aging family#aging life care manager#aging parent care#aging parent crisis#ALCA care Manager#care manager#case manager#celebrations with siblings#Clinical Tools Dysfunctional Holiday#Clinical tools for Mother&039;s Day#dysfunctional siblings#Dysfuntional family on holidays#forgiveness with siblings#geriatric care manager#midlife sibling#midlife siblings#Mother&039;s Day Gift#Mothers Day#Mothers Day celebration with siblings#Mothers Day visit#nurse advocate#nurse care manager#Zoom Call with siblings on Mother&039;s Day
0 notes
Text
falling in love w the sweet gay nurse that treated me after my relapse
#jack my beloved#ed mumbles#i just want 2 cry#also i did manage to go talk to nurses today when i was feeling like dying#n he walked around the carpark with me which was nice#also threw up halfway through my psychiatrist appointment#into my HANDS#it was embarrassing#AND after a bit he asked if he could talk to me again#and i walked into the room and there were like 5/6 people there#the head of nursing doctor therapist some other guy#n they all were asking me how they can help me w my shit and i was like I DUNNO#it was weird haha they let me leave after i sat there looking terrified for a bit#its nice tho bc on monday he told me they couldnt rly help me :((((#cause i clearly have an eating disorder but they dont have an eating disorder unit#and also nobody knows wtf im dealing with cause its not typical at all#so they r trying#he did say i should go home for a bit and then be admitted to an eating disorder hospital tho#which.. yeah ok but also.. they r gonna assume im trying to lose weight#i dont CARE abt my weight i like my weight#i just cant eat okkkkk#i did manage to eat TWICE today tho#not much like 1/3rd of a meal each time but soooo much more than i have been eating#so thats good#disordered eating //#also not my sick brain being like 'if u sh again the nice nurse will treat u again'#IT WAS NICE OK......#im not gonna do it......#i cant anyway im under lock n key for the time being#the psychiatrist asked if i wanted leave again
4 notes
·
View notes
Text
Honestly this semester I let myself go in terms of keeping my nails and toes etc done . I hate that because I let school consume me . And next semester I’m not doing that I’m going to make sure I make time for myself ! May it be : brunch , self care maintenance, gym / working out .
I refuse to keep letting school be first in certain aspects .
I’m truly realizing when I’m not good to myself how can I be to my education ?
Time management is truly my worst concept but I’m going to learn it ASAP .
#self care#maintenance#school#student#studystudystudy#pre nursing#nursing#black girls of tumblr#black woman#blackgirlskillingit#note to self#black twitter#time management#priority#metime#self improvement#self love#beauty#brown beauty
4 notes
·
View notes
Text

Need help with your assignments? Hmu
#essayhelp#law assignments#do my management assignment#academic essay#homework help homework business essay for all homework help business#help with nursing care plan assignment#help with criminal law assignment#essay代写#essays#college algebra#calculus#business law assignment experts#law assignment help#ace attorney#college
2 notes
·
View notes
Text
also you DONT have to be a healthcare worker to be the manager at my new jobs clinic so that was already a huge red flag
2 notes
·
View notes
Text
heyyy babes hru!! dale pa' ya themed kenlos blog and new colour scheme for september be upon ye~ 💜 ☜(  ̄ᴥ ̄ )
#partly inspired by the luces violetas lyrics but also by liz's pretty purple blog theme bc we may be scheming a lil sumn here mwehee >:3#well it's not quite september yet but i change my theme either monthly or whenever a new btr song comes out so yeah. no one cares but yeah#fare thee well pink honey theme </3 i'm gonna miss my adorable showverse kenlos icon the most ngl but i love this one too ;v;#and fun fact my header also happens to be my new pc wallpaper :) rip @ red thanksgiving btr photo though ur still my phone wallpaper ily :(#still not over that first verse/bridge in dale pa' ya btw jfc my boys Served like they did in honey but somehow even slayer???#(typing that made me feel pain. why do i say things. we need a healthy dose of shut the fuck up here nurse)#also ah heckles i'm ace (+ bi + nb) and so have a fair amount of rights to this colour idk i deserve this hajajaj#sorry for personal clutter;; actual posts n stuff after this. come get y'all freshly-squeezed garbage courtesy of this human trashbag lmao#i managed to survive a full hectic week at work and am so close to catching uppp hopefully i could be a little more active nowww#do pretty girl don't speak#will delete#tangent: would be cool if my keyboard stopped autocorrecting pa' to på....struggles of having five languages in gboard man :^/
1 note
·
View note
Text
actually that really annoys me at work when i have to bring attention to an issue bc none of the people who are primarily responsible for it have even noticed it, like i'm literally just a cna
granted during night shift it literally is just the nurses and nurse aides on the floor, so yeah we all do a lot and genuinely do work as a team, but still. like i don't blame anyone necessarily bc i know they are all working hard and do their job right, like tbh they don't have an obligation to go above and beyond. but i personally just can't see a thing and not get involved :/
#we also have a unit clerk at night time usually#so depending on who is working that night they can also be a big help#besides that we have respiratory therapists / phlebotomists / and transporters on the night shift#but they have very specific jobs to do#usually they're very willing to help out the nurses and aides with a specific patient l#like if they are already in the room to give a breathing treatment / draw blood / transfer the patient / etc#but that's just them being nice#during the day time there are doctors roundings / student nurses / nurse managers out on the floor to help care for patients#personal
1 note
·
View note